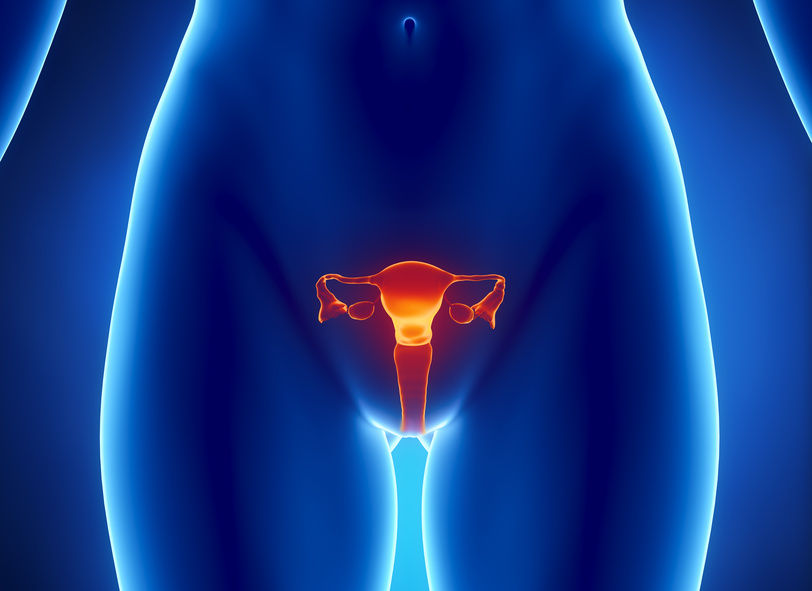
Laparoscopy
If a woman has certain reproductive health issues which affect her ability to conceive, fertility surgery may be an option. Surgery can fix a number of problems including blocked fallopian tubes, endometriosis, fibroids, ovarian cysts and help reduce genetic defects.
A Laparoscopy can help to identify blocked fallopian tubes, as well as myomas, endometriosis and adhesions in the female reproductive organs. During the process, for which a general anaesthetic is necessary, the abdominal wall is pierced with a thin needle. A small camera ensures that the doctor is viewing the organ and can carry out an intervention as appropriate, for which major incisions do not need to be made. However, as is the case in all operations, complications can still occur.
In order to determine whether the fallopian tubes are blocked, a contrast medium is injected into a woman’s body through the vagina. With the aid of the blue dye, the doctors are able to instantly recognise whether the fallopian tubes are permeable. If it was previously discussed with the patient, the doctor can attempt to improve the permeability during the same laparoscopy if necessary. For this purpose, two other small incisions in the pubic region are needed to insert the surgical instruments in the area. Although the laparoscopy is viewed as the best method in the diagnosis of adhesions, it sometimes leads to incorrect results and diagnoses.
www.amitamin.com/en/fertilsan-m New life deserves the best possible start!We provide the essential building blocks for this.
If endometriosis or myomas are detected during the laparoscopy, the doctor can remove them during the procedure, if this was discussed previously with the patient.
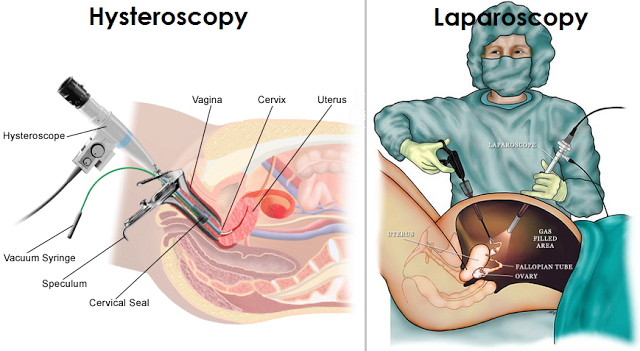
A laparoscopy is also called keyhole surgery. It is the most common type of female fertility surgery. It is minimally invasive and used to both diagnose and treat numerous conditions.
During the procedure, small surgical instruments and devices are inserted into the tummy through small incisions. This helps the surgeon perform whatever surgical procedure needs to be carried out.
It’s often possible to diagnose conditions using non-invasive methods, such as an ultrasound scan, a computerised tomography (CT) scan or magnetic resonance imaging (MRI) scan. Sometimes, however, the only way to confirm a diagnosis is to directly investigate the affected part of the body using a laparoscope, which looks like a metal tube.
Duration
A laparoscopy is usually preformed under general anesthesia and typically takes between half-an-hour and an hour in duration. The length of time will depend on if the procedure is diagnostic or operative. Patients are advised not to drink or eat for at least eight hours prior to having a laparoscopy. Sometimes patients may have to stay overnight, although most patients can go home the same day.
Success Rate
When a woman undergoes fertility surgery for endometriosis or scar tissue her chances of conceiving a child increase to 40-60%. Surgery that clears blocked fallopian tubes has more varying results. These can range from 10 to 90% success rate in conceiving.
Cost
The cost of fertility surgery depends on a number of factors. These include your insurance, the specific operation you are undergoing and where you live. It usually falls in the range of £3,000 to £7,000. The NHS in the UK may cover a laparoscopy, for example to diagnose health problems such as endometriosis. This will require a referral from the GP to a gynaecologist or specialist health clinic.
Side Effects
No surgical procedure is risk-free and recovery times will vary. Directly after the surgery, patients can expect discomfort around the incision(s) site, bloating, cramps, constipation, nausea, and shoulder pain from the gas pumped into the abdominal cavity. These side effects usually only last one or two days. Normally patients can return to daily routines within week.
It’s important to seek medical advice if you experience persistent vomiting and nausea for over 24hrs, bleeding or swelling around the incision site, or fever.
Candidates for laparoscopy
Generally any person that meets the criteria for abdominal surgery is a candidate for laparoscopy. This procedure is unsuitable for patients with significant medical problems or adverse reactions to anaesthesia.

Dr. Kooner is Deputy Director of The Advanced Fertility Center of Chicago and has been a Specialist in Fertility Treatment since 1999.
As well as the areas that the clinic specialises in general, he is particularly interested in managing oocyte donation, female same-sex couples, single women having sperm donation and those considering egg freezing.
Dr. Kooner regularly speaks at fertility meetings. He has published in national journals and constantly contributes to the fertility research and publications from Advanced Fertility Center of Chicago.



