If a couple decides to use artificial fertilisation, a new phase of family planning begins. The process can be financially, physically and mentally demanding on both partners – but the ultimate reward is near.
Women may struggle with the hormones they need to take. These can result in strong mood swings, stomach pains and nausea. This period can be difficult for men as they often feel completely helpless.
In addition, the financial costs can be a big burden on the household budget, as a couple often bears a great deal of expense for fertility treatments.
www.amitamin.com/en/fertilsan-m New life deserves the best possible start!We provide the essential building blocks for this.
Usually the last (but effective) resort
Because of this, couples tend to opt for artificial fertilisation only after all other natural methods of conception have been exhausted.
Men must make sure that their sperm quality is at its highest. This means that they must implement lifestyle changes and boost their diet in a specific way[1]”Morales ME, Rico G, Bravo C, Tapia R, Alvarez C, Mendez JD. Progressive motility increase caused by L-arginine and polyamines in sperm from patients with idiopathic and diabetic … Continue reading,[2]”Scibona M, Meschini P, Capparelli S, Pecori C, Rossi P, Menchini Fabris GF. L-arginine and male infertility. Minerva Urol Nefrol. 1994; 46(4): 251-3″.
A number of micro nutrients have proven to stimulate the development of healthier and more mobile sperm in subfertile men (see comparison on the left).
For women, it is recommended that high doses of multivitamin compounds are taken, which reduce oxidative stress. Vitamins, folic acid [3]”Laanpere M, Altmae S, Stavreus-Evers A, Nilsson TK, Yngve A, Salumets A. Folate-mediated one-carbon metabolism and its effect on female fertility and pregnancy viability. Nutr Rev. 2010; … Continue reading and essential fatty acids should also be included, because these micro nutrients can encourage healthy development of the embryo[4]”Coletta JM, Bell SJ, Roman AS. Omega-3 fatty acids and pregnancy. Rev Obstet Gynecol. 2010; 3(4): 163-171″,[5]”Greenberg JA, Bell SJ, Ausdal WV. Omega-3 fatty acid supplementation during pregnancy. Rev Obstet Gynecol. 2008; 1(4): 162-169″.
Risks
There are a number of obvious risks associated with artificial fertilisation. These can be successfully managed if the couple is well-informed ahead of treatment. Please read our dedicated article by clicking the button below.
Watch our Video Guide
Costs and success chances by artificial fertilisation method
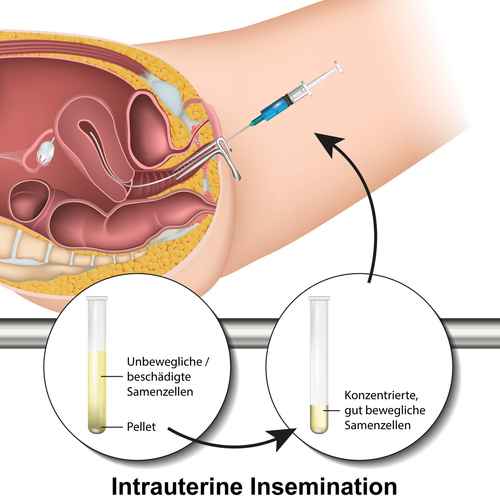
Intrauterine Insemination
Intrauterine insemination (IUI) is the more common method of artificial fertilisation, in which sperm, which laboratory treated sperm is injected directly into the uterus. When only a very small amount of sperm cells is available, a similar method called intratubal insemination (ITI) is used instead. In this case the sperm is injected directly into the fallopian tube.
Sperm is usually obtained through masturbation. The insemination itself is painless and the procedure is not associated with any major risks.
Costs and probabilities of success
If a female uses her partner’s sperm, the average cost of artificial insemination in Western Europe and the United States averages approximately $500 / €400 / £350 per cycle. This cost, however, may rise to $2,500 / €2,000 / £1,750 once you add in the cost of ultrasound monitoring and medication.
Please note that costs should be significantly lower in Eastern Europe and the Far East depending on the institution.
Success rates depend on you and your partner’s fertility profile and your age. Most couples who turn to IUI have a 5 to 20 percent chance of becoming pregnant with each cycle. If fertility drugs are used in conjunction with the procedure chances may be approximately 20 percent. Live birth statistics are not being recorded for artificial insemination.
In-Vitro Fertilisation
In in-vitro fertilisation, the mature egg cells of a woman are removed and combined with the sperm of her partner in a laboratory. If successful fertilisation occurs, up to four embryos (depending on the country) are introduced into the uterus of the woman through the vagina. If more than four egg cells become fertilised, these can be frozen for a later treatment.
Costs and probabilities of success
The HFEA (Human Fertilisation and Embryology Authority) in the UK presents the success chances for both IVF and ICSI in the following way:
A woman’s ability to conceive a child reduces with age. If she is using her own eggs, on average, she has higher chances of success the younger she is.
In the UK in 2010 (the year for which the most recent data is available) the percentage of cycles started, which resulted in a live birth (national averages) in women having in vitro fertilisation using fresh embryos created with their own fresh eggs was:
- 32.2% for women aged under 35
- 27.7% for women aged between 35–37
- 20.8% for women aged between 38–39
- 13.6% for women aged between 40–42
- 5.0% for women aged between 43–44
- 1.9% for women aged 45 and over
The majority of women have per-cycle success rates of 20-35%. That is why up to three cycles are attempted.
Cost can range dramatically from approximately $10,000 / €8,000 / £7,000 per cycle in the USA and in the UK, to approximately $4,500 / €4,000 / £3,500 per cycle in Western European countries like France and Spain, to $2,000 / €1,600 / £1,400 or less in countries like India, Turkey and Lithuania.
Some IVF specific risks
After the transfer of the embryos, the woman may take the corpus luteum hormone progesterone, in order to help support her own body. In these cases the probability of an ectopic pregnancy or a miscarriage is a little higher in IVF than it is in natural fertilisation.
Whether the rate of congenital deformities is higher using these methods of artificial fertilisation is a controversial issue among professionals [6]”Chian RC, Xu CL, Huang JYJ, Ata B. Obstetric outcomes and congenital abnormalities in infants conceived with oocytes matured in vitro. Facts Views Vis Obgyn. 2014; 6(1): 15-18″ has not been conclusively demonstrated.
Intracytoplasmic Sperm Injection
The procedure known as intracytoplasmic sperm injection (ICSI) is very similar to IVF in terms treatment steps and risks involved. In IVF treatment the sperm and egg cells are only combined outside the body ( = “in vitro”) in the test tube, allowing for a natural penetration of the egg by a sperm cell.
For ICSI the doctor injects an individual sperm cell directly into the egg cell. This method is therefore particularly useful in cases where the male’ sperm quality is very low and little or no germ cells are found in his sperm.
Costs and probabilities
ICSI success chances are virtually identical to IVF and therefore not presented separately. Please refer to the probabilities section in the IVF box above.
The cost of ICSI in the USA and UK averages $1,500 / €1,200 / £1,000 per cycle. Expect prices to vary depending on your fertility profile and location.
Prices tend to be estimations based on an approximate 10-12 days fertility drugs stimulation for IVF, ICSI and IMSI treatment cycles. Drug costs are hard to predict as response to stimulation varies from patient to patient and doses may be increased or decreased during the fertility treatment cycle.
Again, both treatment and drug prices are likely to be significantly lower in Eastern European countries or outside of Europe.
ICSI specific risk
A man’s sperm if often obtained for ICSI with the use of tissue extraction from the testes or the epididymis. For the biopsy of the testicles or epididymis, a short-lasting anaesthetic is needed. The microsurgical operation involves a certain level of risk, as is the case with all operations.
Egg Donation (Allogeneic Egg Transplantation)
This process involves an egg cell from a donor being fertilised in a test tube using a man’s sperm. This process is not allowed in several EU countries such as in Germany.
In this form of artificial fertilisation, the fertilised egg cell from the donor is transferred into the uterus of the woman trying to become pregnant. The donor often then abandons any connection with the child on her part.
General cost guidelines
As explained in the individual sections, costs vary greatly and are usually not covered by medical insurance. In general, you should budget no less than $12,000 / €10,000 / £8,000 to be able to expect professional treatment and a realistic chance of success.
Yet, costs should not be your primary concern. More important is your health and the search and selection process for your fertility clinic.
During your selection process, keep the following trends in mind:
- In areas with few infertility clinics, prices, on average, are higher due to less competition
- High cost of living does not equate to high treatment costs
- IUI prices ranged by a factor of 10, i.e. a huge differential. Some quotations included medications, blood work and sonograms; others did not—hence the large price differential.
Questions you should ask
Couples considering artificial fertilisation should choose their clinic carefully and weigh up a number of factors. If cost is a factor in your decision making, ask the clinic for a detailed list of procedures and corresponding costs, and follow up with these questions:
- Are fertility drugs, tests, lab work and consultations included in the cost of treatment?
- Does the clinic provide financial and psychological counseling? If so, are there any additional fees for these services?
- Since most patients do not have insurance coverage for infertility treatment, knowing the costs up front makes good financial sense.
The Fertility Directory
We have a number of clinics and specialists in our database that are highly recommended and have a long history and vast experience in their field.
Please browse here and do not hesitate to contact these specialists with the questions above:
Bibliography

Dr. Kooner is Deputy Director of The Advanced Fertility Center of Chicago and has been a Specialist in Fertility Treatment since 1999.
As well as the areas that the clinic specialises in general, he is particularly interested in managing oocyte donation, female same-sex couples, single women having sperm donation and those considering egg freezing.
Dr. Kooner regularly speaks at fertility meetings. He has published in national journals and constantly contributes to the fertility research and publications from Advanced Fertility Center of Chicago.
References
| ↑1 | ”Morales ME, Rico G, Bravo C, Tapia R, Alvarez C, Mendez JD. Progressive motility increase caused by L-arginine and polyamines in sperm from patients with idiopathic and diabetic asthenozoospermia. Ginecol Obstet Mex. 2003; 71: 297-303 |
|---|---|
| ↑2 | ”Scibona M, Meschini P, Capparelli S, Pecori C, Rossi P, Menchini Fabris GF. L-arginine and male infertility. Minerva Urol Nefrol. 1994; 46(4): 251-3″ |
| ↑3 | ”Laanpere M, Altmae S, Stavreus-Evers A, Nilsson TK, Yngve A, Salumets A. Folate-mediated one-carbon metabolism and its effect on female fertility and pregnancy viability. Nutr Rev. 2010; 68(2): 99-113″ |
| ↑4 | ”Coletta JM, Bell SJ, Roman AS. Omega-3 fatty acids and pregnancy. Rev Obstet Gynecol. 2010; 3(4): 163-171″ |
| ↑5 | ”Greenberg JA, Bell SJ, Ausdal WV. Omega-3 fatty acid supplementation during pregnancy. Rev Obstet Gynecol. 2008; 1(4): 162-169″ |
| ↑6 | ”Chian RC, Xu CL, Huang JYJ, Ata B. Obstetric outcomes and congenital abnormalities in infants conceived with oocytes matured in vitro. Facts Views Vis Obgyn. 2014; 6(1): 15-18″ |







Myy sperms are zero any solution
Dear Shabaz, thank you for your message. You would first need to re-confirm this result by completing a new semen analysis. This will also confirm if there is no sperm present in your seminal fluid, or whether the sperm inside the fluid is dead. We strongly suggest you contact your nearest fertility specialist, Urologist or Andrologist. Once you have been comprehensively diagnosed your specialist will also be able to suggest the best course of treatment. Best of luck!